Knee Pain
Knee Bursitis
- Semimembranosus Bursitis
(Baker's Cyst)
A popliteal cyst, better known as Baker’s cyst, is a fluid-filled swelling that is developed at the back of the knee in the popliteal fossa region.
Ganglia which are benign cystic tumors, originate from synovial tissue. Common areas for cyst can occur at the wrist, hand, foot, and knee.
The cyst can exercise pressure on some anatomical structures, in most cases, the affected anatomical structure is the popliteal vein. Which can develop into thrombophlebitis.
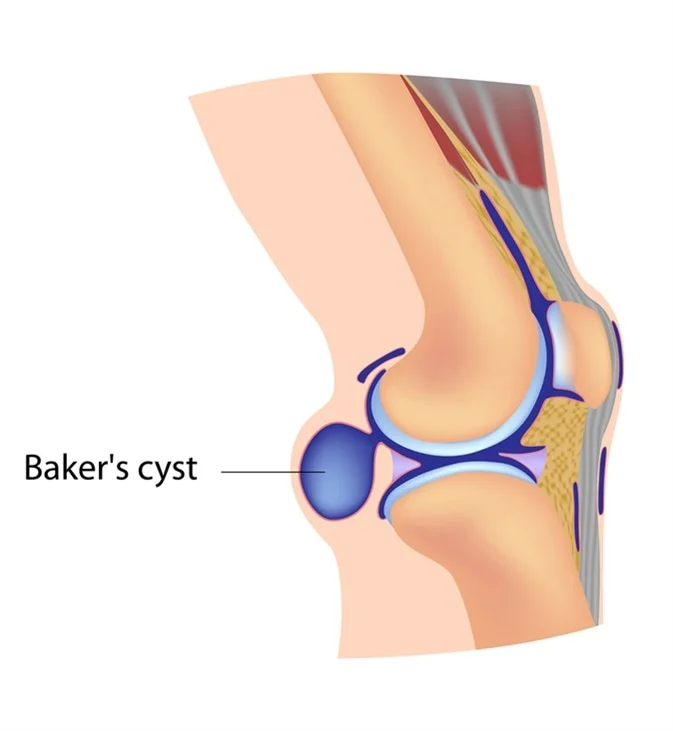
A Bakers cyst is caused by excess fluid in the knee joint. As the joint swells, excess synovial fluid seeps backwards out of the joint and into the popliteal bursa. As the fluid enters the bursa it starts to swell resulting in bursitis.
A number of things can cause the swelling of the knee that leads to a Bakers Cyst:
Osteoarthritis: wear and tear of the knee bones and cartilage leads to increased fluid in the knee joint. 50% of arthritis sufferers develop a Bakers cyst at some point. Osteoarthritis is by far the most common cause of Bakers cysts.
Knee Injuries: any injury that results in swelling inside the knee joint increases the risk of developing a popliteal bursitis. The most common injury to cause a Bakers cyst is a cartilage tear.
Inflammatory Arthritis: There are a few types of inflammatory arthritis that increase the risk of developing a Bakers cyst, the most common being gout.
Symptoms can include:
Vague posterior pain
Swelling and a mass in the popliteal space
Limited range of motion
Stiffness in the back of the knee sometimes increased by activity
Tightness behind the knee
During the physical examination, your doctor will inspect your affected knee and compare it to your healthy knee. They will examine your knee, checking for tenderness, and will also assess the range of motion in your knee and whether pain prevents you from bending it.
Your doctor may employ the following tests:
X-rays. Your doctor may order X-rays to make sure there is not a fracture or other bony problem that is causing your symptoms.
Other imaging tests. The diagnosis of bursitis is usually made on physical examination, but computerized tomography (CT) and magnetic resonance imaging (MRI) scans may be ordered to check for other soft tissue injury.
Aspiration. If your doctor is concerned about the possibility of infection, they may aspirate (draw fluid with a needle) from the bursa and send this sample to the lab for analysis.
There are a number of different treatment options when it comes to a bakers cyst including:
1.Ice
Ice treatment helps to reduce the swelling in the knee and the bursa, which will help to reduce the pain.
In the ice wrap section we look at all the different ways to apply ice and which ones are most effective.
2.Medication
Non-steroidal anti-inflammatory Drugs (NSAIDs) e.g. ibuprofen can help to reduce pain and swelling with popliteal bursitis, but they should only ever be taken on advice of the doctor due to the potential side effects.
3.Stretching Exercises
Tightness in the muscles around the knee aggravates a Popliteal Cyst by squashing it which can lead to further inflammation. Knee stretches can therefore be a very effective way of resolving the condition.
In the Bakers Cyst Stretches section we look at the best exercises to reduce the pressure behind the knee which helps to both treat and prevent further episodes of popliteal bursitis.
4.Aspiration
If a bakers cyst is particularly large or is causing pain behind the knee, then the excess fluid can be drained with a needle by your GP. It is a very simple procedure and usually provides instant relief.
However, it is very common for the fluid to re-accumulate in the bursa if the underlying cause of the bursitis is not address – see Preventing Recurrence below for tips on how to avoid this.
5. Injections
Knee bursitis often responds well to cortisone injections. This is where your doctor injects a mixture of steroid and local anaesthetic into the knee which works to reduce the swelling and reduce the pain behind the knee.
Again, the benefits are usually fairly instant but are often short lived as the swelling returns.
6. Pulsed Electromagnetic Energy (PEME)
Pulsed electromagnetic energy, aka short wave diathermy, is a form of electrotherapy can help to reduce the inflammation.
PEME is usually carried out by a physiotherapist. It can take a few sessions to notice the benefits but I have certainly found this to be an effective treatment with a number of people suffering from a bursitis.
Whilst not usually necessary, in a minority of cases, surgery may be recommended. This is usually the case if the popliteal cyst is a result of long-term damage in the knee e.g. a cartilage tear or arthritis
How using the HeatPulse
and Thermosleeve can help
The Thermosleeve is a cold compression sleeve which can be used to relieve pain and swelling from bursitis or knee surgery. Using the Thermosleeve to ice your knees after activity can also help prevent bursitis.
The Thermosleeve combines cold and compression to numb pain and induce vasoconstriction, bringing down swelling and inflammation. The snug fit around your knee ensures 360 coverage of the injury, boosting the efficacy of the cold therapy.
You may experience pain and swelling in your knee for the first few days after your surgery. Using the Thermosleeve to ice and compress your knee can help relieve these issues.
For the first week after your surgery, use the Thermosleeve at regular intervals 3 or 4 times a day for 10-20 minutes at a time, with at least 30-40 minutes between sessions. After the first week, use the Thermosleeve as needed to relieve pain and swelling.


The Thermosleeve is a cold compression sleeve which can be used to relieve pain and swelling from bursitis or knee surgery. Using the Thermosleeve to ice your knees after activity can also help prevent bursitis.
The Thermosleeve combines cold and compression to numb pain and induce vasoconstriction, bringing down swelling and inflammation. The snug fit around your knee ensures 360 coverage of the injury, boosting the efficacy of the cold therapy.
You may experience pain and swelling in your knee for the first few days after your surgery. Using the Thermosleeve to ice and compress your knee can help relieve these issues.
For the first week after your surgery, use the Thermosleeve at regular intervals 3 or 4 times a day for 10-20 minutes at a time, with at least 30-40 minutes between sessions. After the first week, use the Thermosleeve as needed to relieve pain and swelling.

Hear from customers
who have experienced relief












